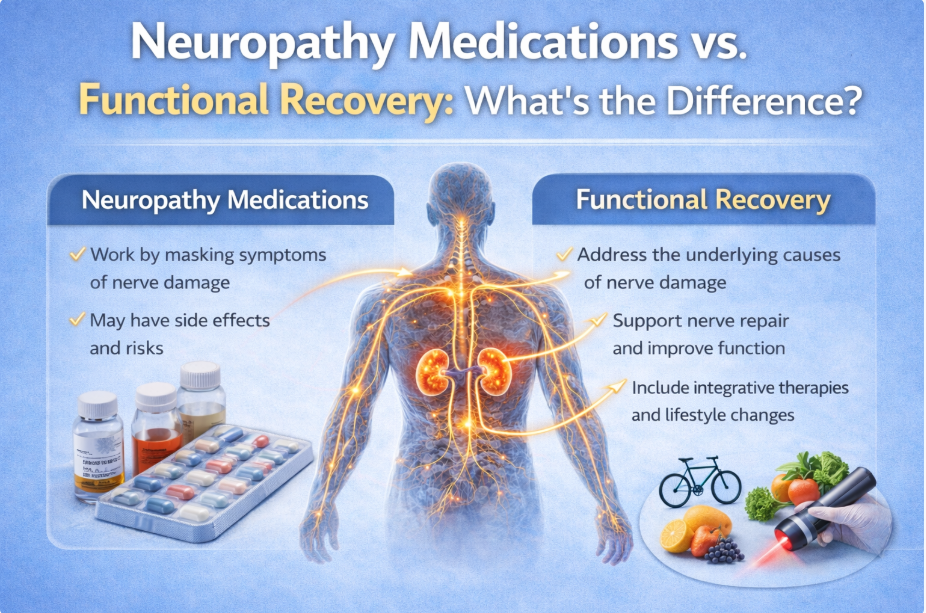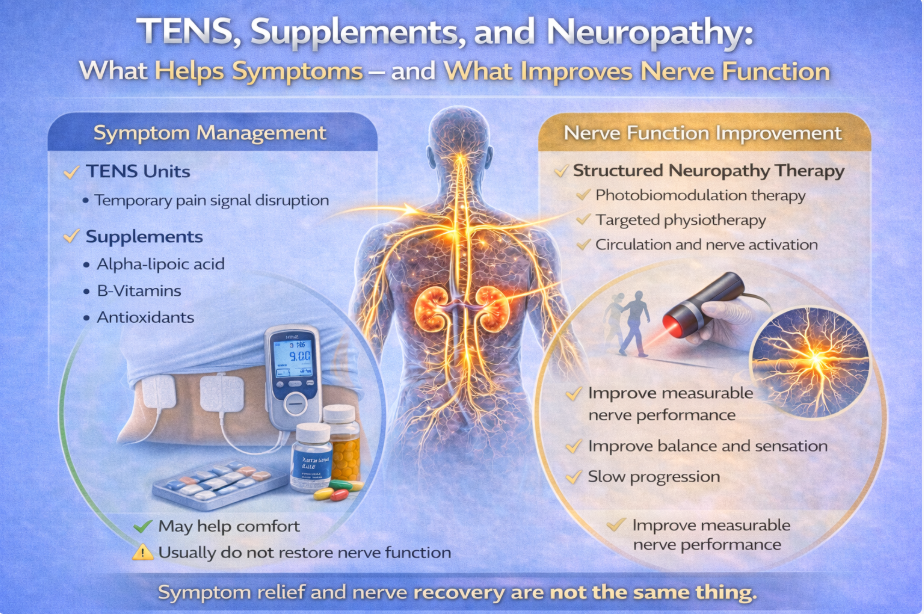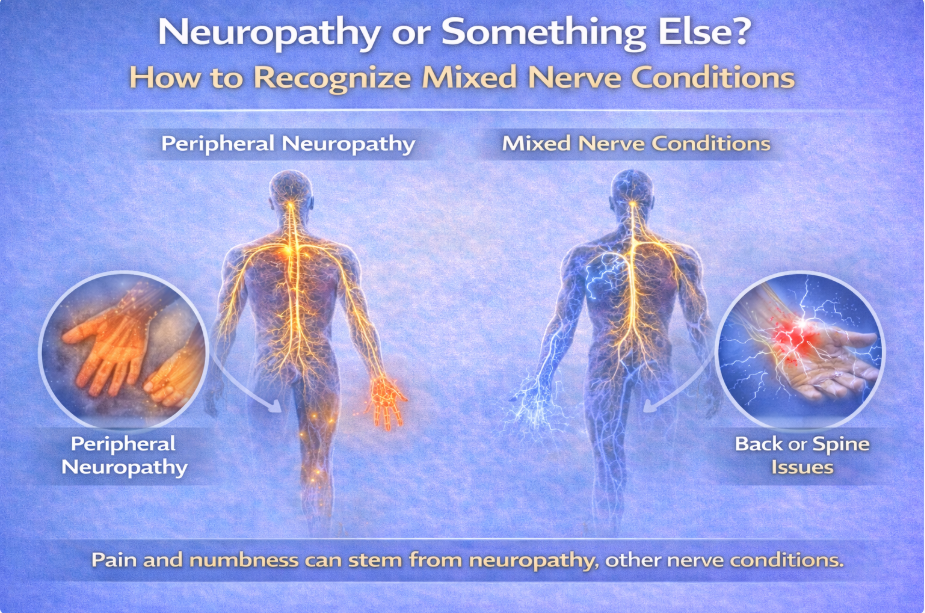
When most people think of peripheral neuropathy, they think of burning, tingling, or numbness in the feet.
But peripheral nerves do more than transmit sensation.
They also regulate automatic bodily functions you rarely think about – heart rate, blood pressure, digestion, sweating, temperature control, and even aspects of tissue regulation.
When these nerves are affected, the condition is called autonomic neuropathy.
And it is frequently under-recognized.
Understanding autonomic involvement changes how symptoms are interpreted – and how care is approached.
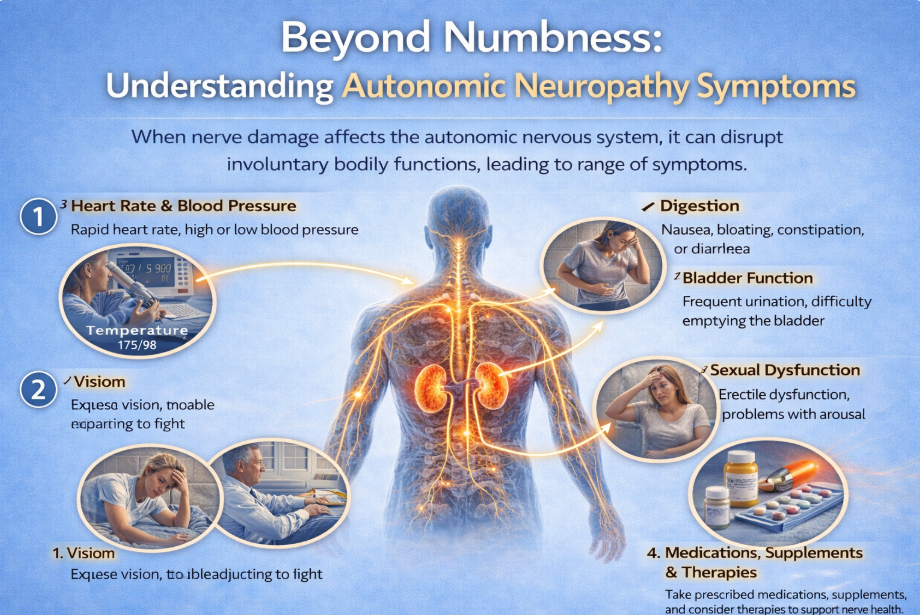
What Is Autonomic Neuropathy?
The autonomic nervous system controls involuntary bodily functions. These include:
- Regulation of heart rate
- Adjustment of blood pressure when standing
- Digestive motility
- Sweating and temperature regulation
- Bladder function
Autonomic neuropathy occurs when these nerves become impaired.
In many patients, autonomic involvement exists alongside sensory neuropathy rather than replacing it.
Medical literature has documented autonomic dysfunction in association with diabetes, chronic kidney disease, autoimmune conditions, and small fiber neuropathy.¹
How Autonomic Symptoms Present
Autonomic symptoms often feel unrelated at first.
Common signs include:
- Lightheadedness when standing
- Rapid or irregular heartbeat
- Digestive slowing or bloating
- Heat intolerance
- Reduced or excessive sweating
- Urinary changes
Because these symptoms span multiple organ systems, they are frequently evaluated separately rather than recognized as neurologically connected.
This fragmentation can delay clarity.
The Overlooked Symptom: Tightness
One of the most common – and least understood – complaints in patients with autonomic and small fiber neuropathy is tightness.
Patients describe it as:
- A band-like constriction in the calves
- A pulling sensation in the arches
- Stiffness that stretching does not resolve
- A constant “wrapped” feeling around the lower legs
This tightness is not simply muscular tension.
Autonomic fibers help regulate vascular tone and microcirculation. When signaling to blood vessels and surrounding tissues becomes dysregulated, tissues may feel chronically restricted or guarded.²
In clinical practice, tightness often becomes a major symptom generator – sometimes even more disruptive than pain.
Standard stretching programs may provide temporary relief but often fail to address the neurological component driving the sensation.
Over more than 20 years focused exclusively on neuropathy care, careful evaluation of sensory and autonomic patterns has proven essential in understanding this symptom.
When tightness is approached methodically rather than mechanically, patients gain clarity about what is truly driving their discomfort.
Why Autonomic Symptoms Matter
Autonomic dysfunction can influence:
- Fall risk (due to blood pressure instability)
- Cardiovascular stability
- Digestive efficiency
- Temperature tolerance
- Overall functional capacity
Loss of blood pressure regulation, known as orthostatic hypotension, is particularly important because it increases fall risk.³
These changes often develop gradually.
Recognition allows earlier intervention and monitoring.
Conditions Commonly Associated With Autonomic Neuropathy
Autonomic involvement is frequently seen in:
- Diabetes
- Chronic kidney disease
- Autoimmune disorders
- Long-standing metabolic dysfunction
- Small fiber neuropathy
In many cases, autonomic symptoms coexist with sensory changes such as burning, numbness, and temperature sensitivity.
Burning feet, tightness, and lightheadedness may share the same neurological origin.
How Evaluation Should Be Structured
Assessment of possible autonomic neuropathy should include:
- Careful symptom history
- Blood pressure measurements when lying and standing
- Review of contributing conditions
- Sensory mapping
- Balance assessment
Autonomic neuropathy rarely exists in isolation.
A comprehensive view of nerve function provides clearer direction than evaluating symptoms individually.
The Most Important Takeaway
Peripheral neuropathy is not limited to numb toes.
When autonomic nerves are involved, symptoms may extend into regulation of blood pressure, digestion, and tissue tone.
Persistent tightness, lightheadedness, or unexplained regulatory changes deserve thoughtful evaluation – not dismissal.
Clarity guides better management.
Frequently Asked Questions
Q: What is autonomic neuropathy?
A: Autonomic neuropathy is nerve damage affecting involuntary bodily functions such as heart rate, blood pressure, digestion, and sweating.
Q: Can autonomic neuropathy cause tightness?
A: Yes. Autonomic dysfunction can alter vascular tone and tissue regulation, contributing to persistent tightness or constricted sensations in the lower legs.
Q: Is autonomic neuropathy serious?
A: It can be, particularly if it affects blood pressure regulation or cardiovascular stability.
Q: How is autonomic neuropathy evaluated?
A: Evaluation may include blood pressure testing, heart rate assessment, neurological examination, and review of underlying conditions.
Next Step
If you are experiencing lightheadedness, digestive slowing, persistent tightness, heat intolerance, or burning and numbness in your feet, a structured neuropathy evaluation can help determine whether autonomic involvement is present.
To learn more or request a consultation at Realief Neuropathy Centers of Minnesota, call 952-456-6160 or submit a request through our website.
Early clarity can influence long-term trajectory.
About the Author
Dr. Timothy Kelm is the founder of Realief Neuropathy Centers of Minnesota and has spent over 20 years focused exclusively on the evaluation and treatment of peripheral neuropathy. He has worked with thousands of neuropathy patients and delivered tens of thousands of neuropathy-focused treatments.
He is associated with published clinical research conducted in collaboration with the University of Minnesota and holds a nationally issued patent related to neuropathy treatment methodology. He has delivered public educational presentations and trained physicians nationally on structured neuropathy care.
Over 20 years ago, his interest in neuropathy began after repeatedly seeing patients who were told there were no good options. He believed then – and continues to believe today – that neuropathy should not define your life.
References
- Vinik AI et al. Diabetic autonomic neuropathy. Diabetes Care.
- Freeman R. Autonomic peripheral neuropathy. Lancet.
- Richardson JK. Peripheral neuropathy and fall risk. Mayo Clinic Proceedings.