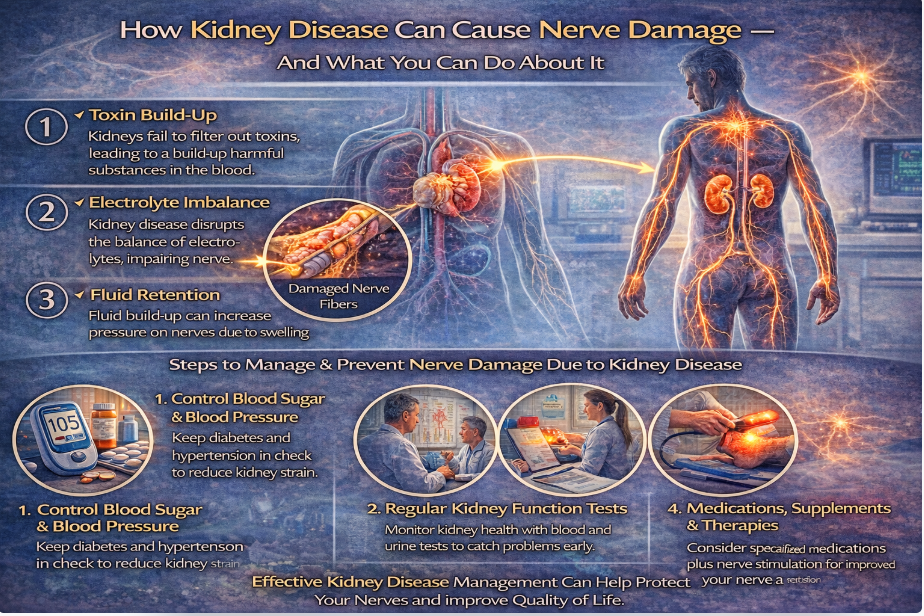
Chronic kidney disease (CKD) affects more than filtration.
As kidney function declines, the nervous system can be affected as well. One of the lesser-discussed complications of advanced kidney disease is peripheral neuropathy, often referred to as uremic neuropathy.
Many patients are educated about dialysis, electrolyte balance, and cardiovascular risks.
Far fewer are told that declining kidney function can directly affect nerve health.
If you are living with chronic kidney disease and noticing burning, numbness, tingling, weakness, balance changes, or unusual tightness in the lower legs, the connection may not be coincidental.
Understanding that relationship matters.
What Is Uremic Neuropathy?
Uremic neuropathy is peripheral nerve damage associated with declining kidney function.
It is most commonly seen in:
- Advanced chronic kidney disease
- Patients approaching dialysis
- Long-standing renal insufficiency
Medical literature has documented peripheral nerve involvement in a significant percentage of patients with advanced CKD.¹
Unlike acute nerve injuries, uremic neuropathy typically develops gradually and symmetrically, beginning in the toes and progressing upward.
Why Kidney Dysfunction Affects Nerves
The relationship between kidney function and nerve health is complex and multifactorial.
Several mechanisms contribute.
1ï¸âƒ£ Accumulation of Uremic Toxins
As glomerular filtration rate (GFR) declines, metabolic waste products accumulate in circulation.
These circulating toxins are believed to contribute to axonal degeneration and impaired nerve conduction.²
Long nerve fibers – particularly in the feet – are especially vulnerable.
2ï¸âƒ£ Microvascular Dysfunction
Chronic kidney disease is associated with vascular changes.
Reduced microcirculatory efficiency may impair oxygen and nutrient delivery to peripheral nerves.
Nerves are metabolically demanding tissues.
When perfusion declines, function often declines with it.
3ï¸âƒ£ Electrolyte and Metabolic Instability
Kidney disease can alter:
- Calcium balance
- Potassium levels
- Acid-base regulation
Subtle but chronic instability may influence nerve excitability and signal transmission.
4ï¸âƒ£ Chronic Inflammation
CKD is associated with systemic inflammatory activation.³
Inflammation is increasingly recognized as a contributor to progressive nerve injury and sensory dysfunction.
What Symptoms Typically Look Like
Uremic neuropathy most often:
- Begins in the toes
- Progresses upward
- Affects both sides
- Develops gradually
Common symptoms include:
- Burning in the feet
- Numbness
- Tingling
- Weakness
- Balance instability
Because progression is slow, many patients normalize early symptoms.
The Role of Tightness in Kidney-Related Neuropathy
Some patients describe persistent tightness in the calves or arches.
This may not simply reflect muscular tension.
Autonomic fiber involvement – which has been described in CKD patientsâ´ – can affect vascular tone and tissue regulation.
When blood vessel regulation and tissue signaling are altered, patients may feel:
- Constriction
- Pulling sensations
- Stiffness that does not respond fully to stretching
Tightness can become a significant symptom driver and is often difficult to treat unless the neurological component is recognized.
Autonomic Involvement in CKD
Kidney-related neuropathy may involve more than sensory fibers.
Autonomic dysfunction can contribute to:
- Blood pressure instability
- Lightheadedness when standing
- Digestive slowing
- Heat intolerance
Autonomic changes are sometimes under-recognized in CKD but are supported in medical literature.âµ
Recognizing these patterns helps prevent misattribution.
Does Dialysis Reverse Neuropathy?
Dialysis reduces circulating toxins.
However, it does not automatically reverse established nerve damage.
Some patients experience stabilization.
Others may continue to notice progression.
Outcomes vary depending on:
- Duration of kidney disease
- Severity of nerve involvement
- Overall metabolic control
Early recognition remains critical.
How Kidney Neuropathy Differs From Diabetic Neuropathy
While symptoms may overlap, their underlying drivers differ.
Diabetic neuropathy is primarily glucose-mediated.
Uremic neuropathy is linked to metabolic waste accumulation, vascular dysfunction, and systemic inflammatory changes.
In many patients, overlapping contributors exist.
Clear evaluation helps determine which factors are dominant.
The Most Important Takeaway
Chronic kidney disease can affect peripheral nerves.
That relationship is well-documented.
But neuropathy associated with kidney dysfunction should not be dismissed as inevitable or untreatable.
Recognition allows:
- Structured monitoring
- Fall risk assessment
- Autonomic evaluation
- Functional tracking
Clarity influences long-term trajectory.
Frequently Asked Questions
Q: Can chronic kidney disease cause neuropathy?
A: Yes. Peripheral neuropathy is a recognized complication of advanced chronic kidney disease due to toxin accumulation, vascular changes, and metabolic instability.
Q: What is uremic neuropathy?
A: Uremic neuropathy refers to nerve damage that develops as kidney filtration declines and metabolic waste accumulates.
Q: Does dialysis cure neuropathy?
A: Dialysis may reduce toxin levels but does not automatically reverse established nerve damage.
Q: What are early signs of kidney-related neuropathy?
A: Early symptoms often include tingling in the toes, burning sensations at night, mild numbness, and subtle balance changes.
Q: Can kidney disease affect autonomic nerves?
A: Yes. Autonomic involvement may contribute to blood pressure instability, digestive slowing, and heat intolerance.
Next Step
If you have chronic kidney disease and are noticing burning, numbness, tingling, weakness, tightness, balance changes, or autonomic symptoms, a structured neuropathy evaluation can help determine whether nerve involvement is present and how it may be progressing.
To learn more or request a consultation at Realief Neuropathy Centers of Minnesota, call 952-456-6160 or submit a request through our website.
Early clarity can influence long-term trajectory.
About the Author
Dr. Timothy Kelm is the founder of Realief Neuropathy Centers of Minnesota and has spent over 20 years focused exclusively on the evaluation and treatment of peripheral neuropathy. He has worked with thousands of neuropathy patients and delivered tens of thousands of neuropathy-focused treatments.
He is associated with published clinical research conducted in collaboration with the University of Minnesota and holds a nationally issued patent related to neuropathy treatment methodology. He has delivered public educational presentations and trained physicians nationally on structured neuropathy care.
Over 20 years ago, his interest in neuropathy began after repeatedly seeing patients who were told there were no good options. He believed then – and continues to believe today – that neuropathy should not define your life.
References
- Krishnan AV, Kiernan MC. Neurological complications of chronic kidney disease. Nat Rev Neurol.
- Bolton CF. Uremic neuropathy. Semin Neurol.
- Arnold R et al. Peripheral nerve dysfunction in chronic renal failure.
- Vita G et al. Autonomic dysfunction in chronic renal failure.
- Mayo Clinic Proceedings. Autonomic neuropathy in systemic disease.